Promoted as a natural, hangover-free substitute toalcoholand available in fashionable cafes and vape stores, the plant-based beverage kava is contributing to a sharp increase in poisonings throughout the United States.
Scientists affiliated with the University ofVirginiaThe Blue Ridge Poison Center reported a 256 percent increase in calls related to kava, rising from 57 in 2011 to 2023 in 2025.
Kava, a plant originating from the Pacific Islands, has been utilized for generations in customary rituals. In the United States, it issold as unregulated concentrated essences, pills, and popular ready-to-drink drinks, frequently marketed as a safe method to unwind without the risks associated with alcohol.
Experts note that the issue lies in strength. Commercial kava products may have two to ten times the amount of active components known as kavalactones, significantly increasing the likelihood of a fast heartbeat, intense vomiting, neurological problems, and liver damage.
The research revealed that the demographic of those being poisoned has also changed. In the early 2000s, most calls centered around young children and women.
Currently, most exposures are among men 20 years old and above, due to the intense advertising of these items close to college campuses and in vape stores, as reported by theCDC
Researchers also noted that kava is becoming more widely usedcombined with kratom, a psychotropic plant with morphine-like effects.
By 2025, kratom accounted for 30 percent of poison center calls related to kava, leading to serious effects such as seizures, high blood pressure, and shaking.

Data from poison centers serves as a preliminary warning system for risks associated with new or resurfacing substances.
After the FDA issued a 2002 warning connecting the substance to liver damage, there was a significant decrease in kava-related reports. However, cases have risen sharply again since 2011.
Dr. Chris Holstege, head of the Blue Ridge Poison Center, stated: ‘We are witnessing a rise in inquiries once more as new kava items become available on the market, including blends with other ingredients like kratom that may lead to negative reactions.’
The document, released by the CDC’sMorbidity and Mortality Weekly Report, depended on data from the National Poison Data System, which gathers details from all 53 U.S. poison centers.
Every time an individual contacted a poison center regarding a potential kava exposure, whether it involved a child who ingested something by mistake or an adult who consumed an excessive amount, the call was recorded in the database.
The group reviewed all calls related to kava that occurred from January 2000 to December 2025, covering a span of 25 years.
For every incident, they documented the individual’s age and gender, if kava was consumed alone or in combination with other substances, the symptoms experienced, the severity of the result, and if hospitalization was required.
They subsequently monitored the evolution of call numbers over the years, identified the callers, and assessed whether results were becoming more or less serious.

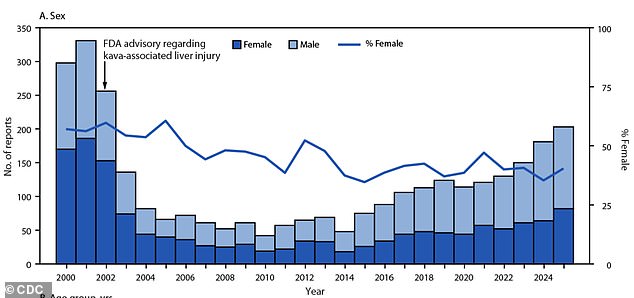
Severe consequences involved life-threatening conditions, hospital admission, or substantial impairment.
From 2000 to 2025, toxicology centers recorded 3,101 calls related to kava. Prior to the FDA’s liver-related alert in 2002, the number of calls was significant — 331 in 2001 — and then dropped by 87 percent to a minimum of 42 in 2010.
The next year saw an increase in reports. The market recovered through new product forms, vigorous wellness advertising, and broader access, which directly contributed to the rise in poison center calls.
The categories of individuals making calls also changed. In the 2000s, women and young children constituted the majority of cases, but by 2025, women accounted for 40 percent of calls and children under 12 represented only seven percent.
Adults aged 20 and above consistently made up approximately two-thirds of all submissions.
More severe consequences have become increasingly frequent. In 2000, just 12 percent of kava exposures resulted in significant health issues.
By 2024, the number had risen to 39 percent. There were eight fatalities recorded during the 25-year span.
Single-substance kava exposure usually led to vomiting, sleepiness, dizziness, and an increased heart rate. However, when kava was mixed with kratom, as occurred in 128 instances, the outcomes were more severe, such as seizures, shakiness, and elevated blood pressure.
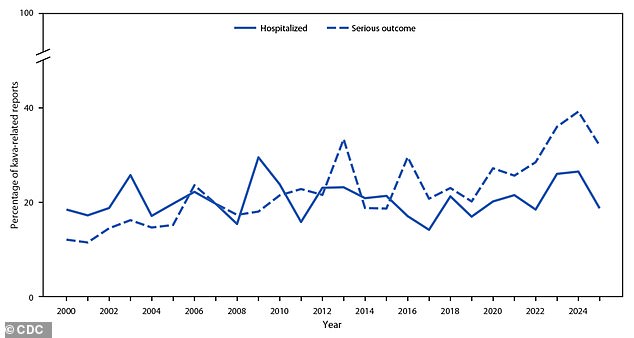
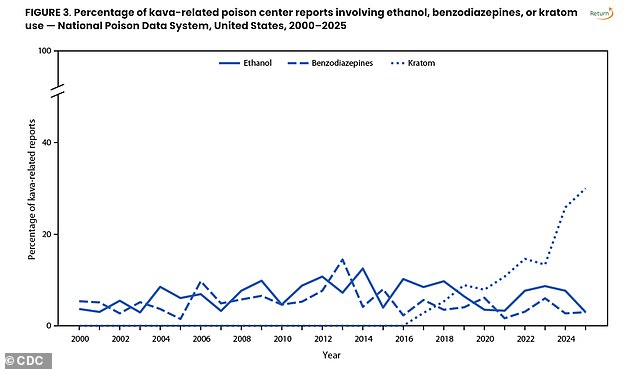
Elevated liver enzymes were also more frequently observed when combining kava and kratom compared to using kava by itself.
An increase in poison center calls related to kava reflects the larger growth in nonalcoholic drinks, as more individuals seek out alcohol-free options.
These items are frequently available online and in vape stores, and they are promoted as a method to experience social interaction without the discomfort of a hangover, which may account for why young adults now represent the largest portion of exposure cases.
Holstege stated: “These new kava products are available in stores across our region.”
The general population should be informed about possible issues that can arise from using these items.
In contrast to other nations that impose limits on kava consumption — such as Australia, which restricts daily intake to 250 mg of kavalactones — the United States does not have similar rules.
Kava and kava-kratom products remain entirely without regulation in the United States, although certain producers claim over 250 mg of active components in a single 30 ml portion, typically offering several servings per package.
Due to the absence of a uniform production or content checking process, the real strength might be even greater.
Medical professionals caution that long-term consumption of these strong formulations has been associated with liver injury, convulsions, increased heart rate, and elevated blood pressure.
As stated by the researchers: ‘Ongoing marketing of these items without proper confirmation of their composition, informing consumers about possible negative health impacts, and awareness among medical professionals about changing exposure trends poses a continuous public health issue.’






Leave a comment