- Expert insights, anti-aging advice, and more! Subscribe to the Your Health newsletter for free HERE
For the first time, researchers have directly observed protein clusters in the brain thought to cause Parkinson’s disease, advancing their efforts toward possible therapies.
Parkinson’s is a progressive, untreatable neurological condition that impacts the brain and has broader effects on the body, significantly affecting the lives of millions.
Individuals often experience worsening tremors and mobility issues that may ultimately lead to a loss of self-reliance.
Although researchers have been aware for many years that small clusters—referred to as alpha-synuclein oligomers—are probably responsible for initiating Parkinson’s disease in the brain, they have not previously been able to observe these proteins within human brain tissue.
But in a significant advancement, specialists from theUniversity of Cambridge, University College London, the Francis Crick Institute and Polytechnique Montreal have created a method that enables them to not only visualize these clusters in the brain, but also quantify them.
For more than 100 years, physicians have diagnosed Parkinson’s disease based on the existence of significant protein accumulations, referred to as Lewy bodies. However, current specialists suggest that these smaller clusters, which develop earlier, could be responsible for the harm to brain cells linked with Parkinson’s.
Professor Steven Lee, an expert in biophysical chemistry at Cambridge and co-lead author of the study, stated: ‘Lewy bodies are the characteristic feature of Parkinson’s, but they essentially indicate where the disease has already affected, rather than where it is currently occurring.’
If we are able to detect Parkinson’s in its initial phases, it would provide significant insights into how the disease progresses in the brain and potential ways to address it.
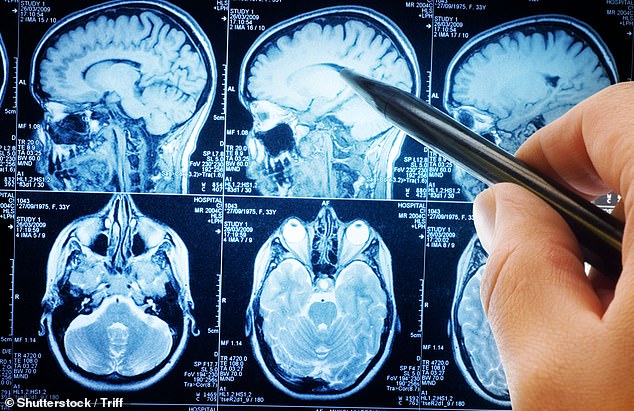
Up until this point, these oligomers were too tiny to observe, measuring just a few nanometres in length, but the research group has recently created a method known as Advanced Sensing of Aggregates for Parkinson’s Disease (ASA-PD) that employs lasers to label proteins in brain tissue obtained after death.
Dr. Rebecca Andrews, who conducted the laboratory study, stated: ‘This is the first time we have been able to examine oligomers directly within human brain tissue at this level: it’s akin to observing stars in full daylight.’
‘Oligomers were like needles in a haystack, but now that we’ve located them, this could enable us to focus on particular cell types in specific areas of the brain,’ said Professor Lucien Weiss, co-lead author of the study, from Polytechnique Montreal.
In the present research, featured in the journalNature Biomedical Engineering,Scientists initially examined brain tissue samples from individuals diagnosed with Parkinson’s disease and contrasted them with those from healthy people of comparable age.
Although the proteins were found in both healthy and Parkinson’s brains, in patients with Parkinson’s, the oligomers were significantly larger, more intense, and present in greater numbers—indicating a clear connection to the disease’s advancement.
The group also discovered a type of oligomers that were present exclusively in individuals with Parkinson’s, which specialists believe might serve as the first detectable signs of the condition—possibly several years prior to the onset of typical symptoms.
“This approach offers more than just a momentary view,” said Professor Weiss.
It presents a comprehensive map of protein alterations throughout the brain, and comparable techniques might be utilized for other neurodegenerative conditions such as Alzheimer’s and Huntington’s.
Professor Sonia Gandhi, a specialist in neurodegenerative diseases at The Francis Crick Institute, stated: ‘The only genuine method to comprehend what occurs in human illness is to examine the human brain directly, yet due to the brain’s immense complexity, this presents significant difficulties.’
Scientists now anticipate that this advancement will promote a deeper comprehension of the reasons, locations, and mechanisms behind the formation of these protein clusters and their role in causing illness.
Typically, a diagnosis is made once later-stage symptoms appear, following the exclusion of other possible health issues.
Parkinson’s charities estimate Over 25% of individuals suffering from the condition receive an incorrect diagnosis prior to receiving the accurate one.
Approximately 166,000 individuals in the UK are believed to be affected by this severe condition, with the figure increasing. By 2050, the global number of Parkinson’s patients is projected to double, reaching an astonishing 25 million.
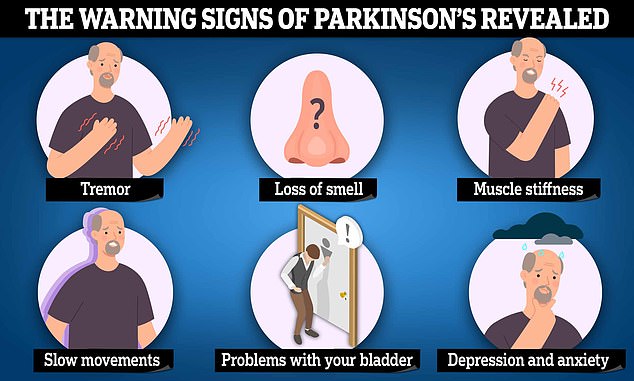
Initial indicators of Parkinson’s disease may consist of a tremor, rigidity, slowed movement, and a diminished sense of smell.
Other typical symptoms include difficulties with balance, coordination, and muscle spasms.
Individuals may also experience mental health issues such as depression and anxiety as a result of their illness.
Although there are medications that can ease certain symptoms resulting from the loss of dopamine-producing brain cells, there are currently no drugs capable of slowing or halting the progression of the disease.
Scientists continue to investigate what causes the demise of these nerve cells.
Nevertheless, modern perspectives suggest it results from a mix of genetic modifications and external influences.
The likelihood of acquiring the condition generally rises with age, as the majority of cases are identified in individuals over 50.
- Valuable insights, anti-aging advice, and more! Subscribe to the Your Health newsletter for free HERE.
- Is Parkinson’s a non-fatal yet life-changing condition quietly affecting 150,000 people in Britain?
- Prepared to fight Parkinson’s through a minor change in daily habits? Discover how everyday dietary decisions could be the solution for avoiding the disease.
- Can obesity and high blood pressure be unknowingly increasing your chances of developing Parkinson’s Disease? A surprising new study reveals modifiable factors linked to this concerning 40% higher risk!
- Can recognizing the initial indicators of Parkinson’s disease prevent later hardship? Learn about the mild symptoms you should be aware of today.
- Why is Parkinson’s disease now the fastest-growing neurological condition, impacting more than a million Americans without any available treatment?





Leave a comment